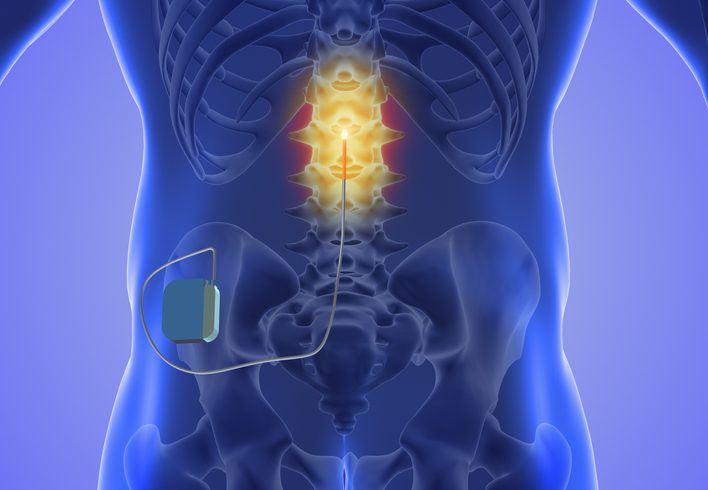
Experiencing sciatica pain can be both physically and emotionally draining. As you navigate the healing process, it’s crucial to understand the journey ahead. The last stages of recovery are a testament to your resiliency and patience, and knowing what to expect can help you stay motivated and focused on regaining your full health.
In this comprehensive guide, we’ll delve into the last stages of sciatica recovery, explore signs of improvement, and discuss valuable strategies for preventing relapse. Moreover, we will examine various treatment options for persistent cases and offer guidance on when to seek professional help.
Key Takeaways
- Understanding the last stages of sciatica recovery is essential for setting realistic expectations and achieving a successful outcome.
- Monitor decreased pain intensity, increased range of motion, and reduced numbness/tingling sensations as signs your sciatica is improving.
- Seek professional help if symptoms worsen or impact daily life to ensure proper recovery from a herniated disc.
Understanding the Last Stages of Sciatica Recovery
As the saying goes, “slow and steady wins the race.” This adage holds for the last stages of sciatica recovery, where patience and perseverance are key. During these final stages, you’ll focus on nerve rehabilitation, regaining strength and mobility, and addressing emotional well-being, allowing you to overcome this challenging episode and return to your normal life.
Specifically, the key steps in sciatic nerve rehabilitation and desensitization include:
- Mitigating inflammation and irritation, which are primary sources of discomfort.
- Helping the sciatic nerve heal and alleviate pain, numbness, and tingling sensations in the affected leg.
- Restoring strength and mobility to resume daily activities without pain.
- Managing emotional well-being and developing coping strategies to stay resilient and focused during the recovery period.
By following these steps, you can effectively recover from sciatic nerve pain and regain your quality of life.
Grasping the final stages of sciatica recovery is imperative to set realistic expectations and ward off potential setbacks. By learning about the various aspects of this process, you can be better prepared for what lies ahead and work towards a full recovery with confidence.
Nerve Rehabilitation and Desensitization
In the fight against sciatica, nerve rehabilitation and desensitization significantly contribute to the final stages of recovery. These processes help reduce sensitivity and prevent future injuries. As your sciatic nerve heals and inflammation decreases, the surrounding muscles become less restrictive, allowing for a greater range of motion, which is a sign of healing and progress in recovering from sciatica.
Working closely with healthcare professionals, such as physical therapists, can help you navigate the complexities of nerve rehabilitation and desensitization. They can provide:
- Tailored treatment options
- Manual therapy techniques
- Support for the healing process
- Guidance towards a full recovery
Regaining Strength and Mobility
Rebuilding strength and mobility is vital for complete recovery from sciatica and getting back to daily activities. The objective is to strike a balance between physical activity and inactivity, preserving flexibility and strength without exacerbating the sciatica or leading to further injury.
Increased range of motion is a positive sign of sciatica recovery. As you advance in your healing journey, partnering with a physical therapist who can guide you through suitable exercises tailored to your needs and limitations is key. These exercises not only help restore strength and mobility but also prevent sciatica from recurring.
Remember, patience is vital during this phase of recovery. Pushing yourself too hard or too soon can lead to setbacks and further complications. Be sure to consult with a healthcare professional to ensure you’re on the right track to get better, towards getting better and staying pain-free.
Emotional Well-being and Coping Strategies
The emotional impact of sciatica is immense. Chronic pain, diminished mobility, and the strain of managing a continuous condition can result in psychological distress and depression. Addressing your emotional wellness during the final stages of recovery is vital, as it significantly factors into your overall healing process.
Mindfulness techniques, such as deep breathing exercises and meditation, can help manage the emotional stress caused by sciatica. Moreover, support from friends, family, and healthcare professionals can provide a valuable network of encouragement and understanding throughout your recovery journey.
By acknowledging the emotional challenges and seeking appropriate support, you can maintain a positive mindset and stay resilient in your path towards full recovery.
Signs Your Sciatica is Improving
As you advance in your recovery journey, it’s vital to identify the markers of your improving sciatica. These indicators can provide reassurance, motivation, and a sense of accomplishment, knowing that your efforts are paying off.
Decreased pain intensity and frequency, increased range of motion, and reduced numbness and tingling sensations are all signs that your sciatica is getting better. By staying vigilant and monitoring your progress, you can ensure that you’re on the right track towards a full recovery and a pain-free life.
Decreased Pain Intensity and Frequency
One of the most crucial indicators of sciatica improvement is a decrease in pain intensity and frequency. This suggests that the sciatic nerve is on the path to recovery and inflammation is reducing.
Generally, sciatica pain lasts between 2-6 weeks, with acute pain gradually decreasing. Most cases of sciatica resolve within 4-6 weeks with conservative or no treatment. However, if the pain is severe or persists for more than 6 weeks, it is advisable to seek medical advice for treatment options.
It’s important to monitor your pain levels throughout your recovery journey, as this information can help you and your healthcare provider determine the most effective treatment options and ensure that you’re progressing as expected.
Increased Range of Motion
An increase in range of motion is another sign of sciatica improvement. As the sciatic nerve heals and inflammation decreases, the surrounding muscles become less tight and restrictive, allowing for a greater range of motion.
This increased mobility is a sign of healing and progress in recovering from sciatica. It can also help to strengthen muscles, improve joint mobility, and enhance the adaptability of the nervous system. Massage therapy and physical therapy exercises are some activities that can help to increase range of motion and promote healing.
Reduced Numbness and Tingling Sensations
Reduced numbness and tingling sensations are another indication that your sciatica is improving. This signifies that nerve function is gradually returning to normal.
Generally, it can take between four to twelve weeks for numbness and tingling sensations to reduce in sciatica recovery. The stages of nerve recovery associated with the reduction in numbness and tingling in sciatica patients may differ depending on the individual and the severity of their condition. Nevertheless, some common stages of nerve recovery include:
- Inflammation reduction
- Nerve healing
- Numbness and tingling reduction
- Full recovery
By monitoring the reduction of these symptoms, you can ensure that you’re on the right path towards a full recovery and a pain-free life.
Preventing Sciatica Relapse
Preventing sciatica relapse is a crucial aspect of your long-term recovery plan. By maintaining good posture, engaging in regular exercise and stretching, and making necessary lifestyle modifications, you can reduce the risk of future sciatica episodes and maintain a pain-free life.
This section will delve into different strategies for averting sciatica relapse, equipping you with valuable methods to protect your progress and uphold your overall spinal health.

Maintaining Good Posture
Upholding good posture is a key strategy for averting sciatica relapse. Good posture helps maintain spinal alignment and reduces the risk of nerve compression, which can lead to sciatica.
By being mindful of your posture during daily activities, such as sitting at a desk, standing, and lifting objects, you can reduce strain on your lumbar spine and prevent sciatica from recurring. Ergonomic chairs that support the lower back can also help promote proper posture and reduce the risk of spinal stenosis and sciatica relapse.
Regular Exercise and Stretching
Consistent exercise and stretching form a crucial part of preventing a recurrence of sciatica. Engaging in physical activity can help improve muscle strength, flexibility, and overall spinal health, reducing the risk of future sciatica episodes.
A variety of exercises, including gentle aerobic activities like walking and swimming, can help maintain spinal health and prevent sciatica relapse. In addition, stretching exercises targeting the lower back, hips, and legs can improve flexibility and reduce muscle tension, further reducing the risk of sciatica recurrence.
Remember to consult with a healthcare professional or physical therapist to determine the appropriate exercise and stretching regimen for your specific needs, as this can ensure that you’re engaging in activities that support your long-term recovery and spinal health.
Also Read: 9 Effective Sciatica Exercises for Pain Relief
Lifestyle Modifications
Lifestyle modifications, such as weight management and ergonomic adjustments, can play a significant role in preventing sciatica relapse. Some tips for preventing sciatica relapse include:
- Maintaining a healthy weight through exercise and a balanced diet
- Avoiding prolonged sitting or standing in one position
- Using proper posture and body mechanics when lifting heavy objects
- Incorporating regular stretching and strengthening exercises into your routine
- Using ergonomic furniture and equipment to support your spine and reduce strain
By implementing these lifestyle modifications, you can help reduce inflammation, lower the risk of developing sciatica, and prevent future relapses.
Ergonomic adjustments at home and work can also help prevent sciatica relapse by reducing pressure on the nerves and soft tissues in the lower back. Suggested tips include:
- Maintaining an upright posture
- Evenly distributing weight
- Utilizing ergonomic furniture that supports the lower back
- Modifying postures and activities to relieve pressure
Treatment Options for Persistent Sciatica
In certain instances, sciatica may continue even with your utmost efforts to control symptoms and foster healing. If you find yourself struggling with persistent sciatica, it’s essential to explore various treatment options to ensure a proper recovery.
Physical therapy, medication management, and alternative therapies are all potential treatment options for persistent sciatica. This section will examine each of these approaches, offering valuable insights to help you identify the most appropriate path for your unique situation.
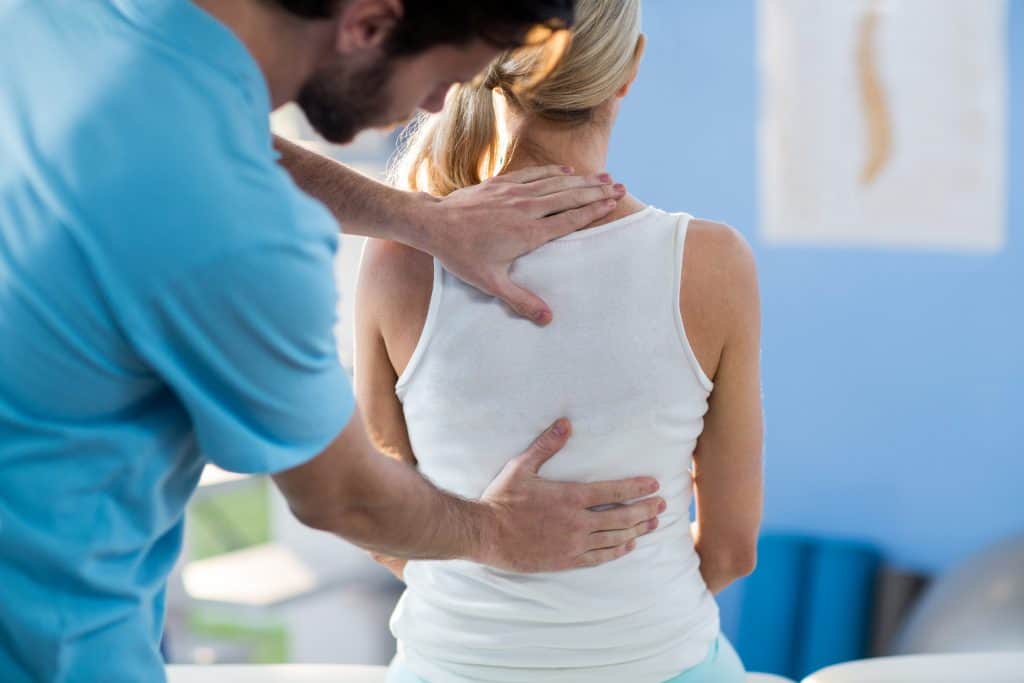
Physical Therapy
Physical therapy is a highly effective treatment option for persistent sciatica. It helps improve strength, flexibility, and posture, addressing the root cause of sciatica and promoting long-term recovery.
Working with a physical therapist can help you:
- Develop a tailored exercise and stretching regimen that targets your specific needs and limitations
- Release tension in the sciatic nerve
- Alleviate muscle spasms that may be contributing to your pain
The duration of physical therapy for sciatica recovery varies, but it generally ranges from 4 to 12 weeks or longer, depending on your individual case. By committing to a physical therapy program, you can improve your overall spinal health and reduce the risk of future sciatica episodes.
Medication Management
Medication management is another treatment option for chronic sciatica. Pain relievers, anti-inflammatory drugs, and muscle relaxants can help alleviate sciatica symptoms and support your recovery.
The type and duration of medication use can vary depending on your specific situation and the severity of your symptoms. It’s important to consult with your healthcare provider to determine the most appropriate medications for your needs and to ensure that you’re using them safely and effectively.
Alternative Therapies
Alternative therapies, such as acupuncture, massage, and chiropractic care, can provide additional pain relief and support the healing process for those struggling with persistent sciatica.
Acupuncture has been shown to:
- Relax tight muscles
- Improve blood circulation
- Regulate the nervous system
- Reduce inflammation
These benefits can provide relief from sciatic pain and help with sciatica get better.
Similarly, massage therapy has been demonstrated to provide temporary relief from pain and discomfort associated with sciatica.
Keep in mind that the potential side effects and complications of alternative therapies can vary from person to person, and it’s crucial to consult with a healthcare professional before pursuing any alternative treatments.
When to Seek Professional Help
Recognizing when to seek professional assistance for sciatica is vital to guarantee appropriate treatment and recovery. If your symptoms worsen, your pain becomes unmanageable, or your daily life is significantly impacted, it’s crucial to consult with a healthcare professional for guidance and support.
This section will explore particular scenarios where professional intervention may be necessary and give guidance on when to seek help for effective sciatica management.
Worsening Symptoms
Worsening symptoms may indicate an underlying issue that requires further evaluation and treatment. If you experience:
- moderate to severe pain
- numbness and tingling
- muscle weakness
- alterations in bowel and/or bladder control
It’s essential to seek professional help.
Failure to obtain professional assistance when experiencing sciatica pain can result in:
- Delayed recovery
- Permanent disability
- Nerve damage
- Heightened pain and discomfort
By seeking help early on, you can ensure that you receive the appropriate treatment and support for your specific needs.
Inability to Manage Pain
If your sciatica pain becomes unbearable or unmanageable with self-care measures, making your sciatica worse, it may be necessary to seek professional intervention to ensure proper recovery from a herniated disc.
Severe or intolerable back pain, including sharp pain, that hinders daily activities and quality of life, bilateral pain, or pain resulting from a direct injury to the back are all indications for professional intervention in the case of unmanageable sciatica pain. By seeking help, you can receive the necessary guidance and support to manage your pain and promote recovery, especially if it’s related to degenerative disc disease.
Impact on Daily Life
If sciatica significantly impacts your daily life, it’s essential to seek professional help. Sciatica can interfere with work, family responsibilities, and overall quality of life, making it challenging to carry out your daily activities.
In addition to the physical limitations, sciatica can also adversely affect your mental well-being and personal relationships. By seeking professional help, you can receive the necessary guidance and support to manage your pain, reduce its impact on your daily life, and promote a full recovery.
Summary
Navigating the challenging journey of sciatica recovery can be daunting, but understanding the various stages, signs of improvement, and strategies for prevention and treatment can provide valuable guidance and support. By following the advice outlined in this comprehensive guide, you can stay motivated, focused, and confident in your path towards a full recovery and a pain-free life.
Remember, every individual’s experience with sciatica is unique, and your recovery journey may look different from someone else’s. Stay patient, persevere, and seek professional help when needed. With the right approach and mindset, you can overcome this challenging period and emerge stronger and more resilient.
Frequently Asked Questions
How do you know when sciatica is ending?
As sciatica ends, you may notice that the pain and discomfort have become less severe. You might experience fewer flare-ups, or find it easier to move between seated and standing positions. In some cases, however, the sciatica will not go away.
What are red flags for sciatica?
Red flags for diagnosing sciatica include pain that is limited to one side of the body, radiating pain down the leg, and pain when standing or sitting.
What is the longest time sciatica can last?
With proper care and treatment, acute sciatica symptoms typically don’t last longer than four to eight weeks. Most healthcare experts agree that sciatica should go away on its own with the right treatment, and data shows that about half of people recover within six weeks.
What is the cause of sciatic nerve pain?
Sciatica is caused by pressure or damage to the sciatic nerve, resulting in pain radiating from the lower back or buttock down the leg. Common causes include herniated discs, lumbar spinal stenosis, degenerative disk disease, and overgrowth of bone spurs on the spinal bones, as well as tumors or diseases that can damage the nerve.
What are some effective exercises for sciatica relief?
Effective exercises for sciatica relief include Clamshell, Press-Up Exercise, Isometric exercises, Abdominal sets, and Hip Flexor Stretch. Be sure to consult with a physical therapist to create a personalized exercise plan.