Sacroiliac joint fusion is a surgical procedure aimed at relieving pain and stabilizing the SI joint, which connects the spine to the pelvis. Commonly employed when non-surgical treatments for SI joint dysfunction fail to provide relief, this surgery involves the fusion of the sacroiliac joint to eliminate motion and alleviate the associated discomfort. Patients with chronic pain resulting from conditions such as abnormal SI joint movement or degenerative sacroiliitis often consider this procedure as a means to regain function and improve quality of life.
Understanding the anatomy and biomechanics of the sacroiliac joint is essential, as it plays a significant role in transferring weight and movements between the upper body and legs. Disruptions in its function—be it excessive motion (hypermobility) or stiffness (hypomobility)—can lead to debilitating symptoms affecting daily activities. Sacroiliac joint fusion surgery is a complex process that requires a comprehensive diagnosis and careful consideration of all treatment options, including potential risks and the rehabilitation process to ensure the best possible outcomes.
Key Takeaways
- SI joint fusion is a last-resort procedure to alleviate pain and stabilize the sacroiliac joint when other treatments fail.
- Proper diagnosis of SI joint dysfunction is crucial for the success of surgical intervention.
- A full recovery includes a careful rehabilitation process following the surgery to restore function.
Anatomy of the Sacroiliac Joint
The sacroiliac joint (SI joint) is a critical link between our spine and pelvis, providing stability and supporting the weight of the upper body. Composed of the sacrum and the ilium, this joint is reinforced by a network of strong ligaments and minimal cartilage.
The sacrum, a triangular bone at the base of the spine, interlocks with the ilium – part of the pelvis – to form the sacroiliac joint on both sides of the body. These joints are designed to be relatively immovable, allowing only slight, cushioned movements to absorb shock between the upper body and the lower extremities.
Here’s a quick glance at the SI joint structure:
- Articulating Bones: Sacrum and Ilium
- Joint Type: Synovial (limited movement)
- Ligaments:
- Anterior sacroiliac
- Interosseous sacroiliac
- Posterior sacroiliac
The interior of the joint is lined with synovial membrane and contains fluid that lubricates and minimizes friction during the slight movements that occur. The surfaces inside the joint have jagged edges which, along with the ligaments, restrict movement for added stability.
Our understanding of the SI joint’s anatomy provides insight into its important role in connecting our spine to our lower body, affecting our ability to stand and walk. In-depth knowledge of this anatomy is vital, especially when considering treatments like SI joint fusion to alleviate pain stemming from joint dysfunction.
Causes of Sacroiliac Joint Dysfunction
We understand that sacroiliac joint dysfunction is often the result of specific conditions that affect the joint, altering its normal function and causing pain. Let’s examine the primary causes that contribute to this problem.
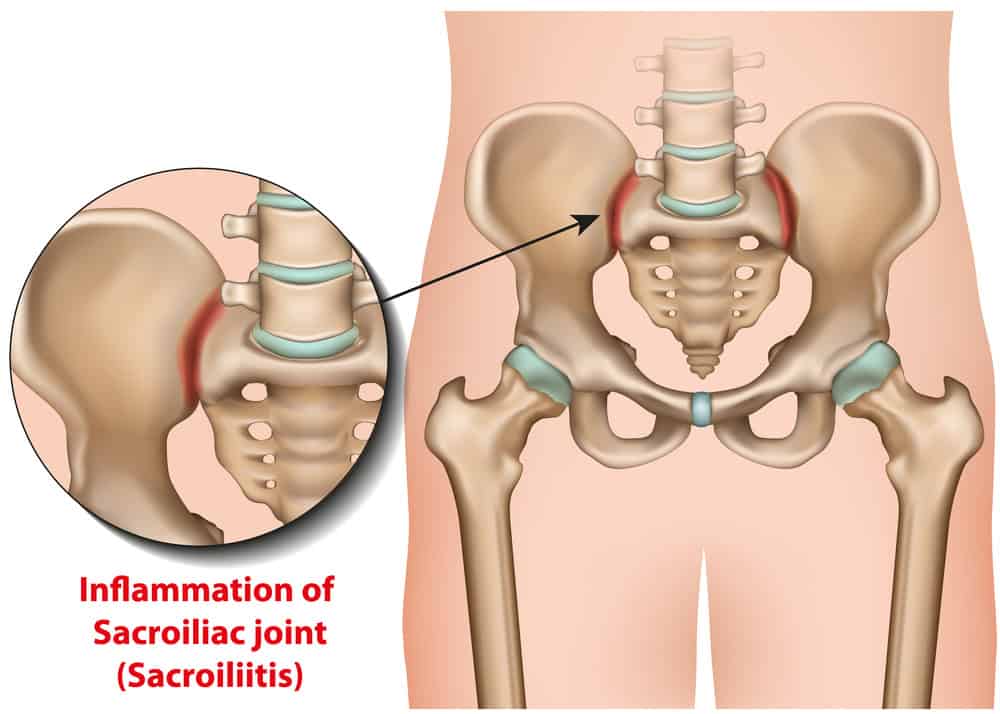
Arthritis
Arthritis significantly impacts our joints, and the sacroiliac joint is no exception. Osteoarthritis can develop due to age-related wear and tear on these joints. Ankylosing spondylitis, a type of inflammatory arthritis that affects the spine, can also lead to dysfunction in the sacroiliac joints. These forms of arthritis cause a degeneration of the joint, which in turn can lead to altered movement and chronic pain.
Pregnancy
Pregnancy introduces a unique stress on the sacroiliac joints. During this time, our bodies release a hormone called relaxin, which causes ligaments to relax in preparation for childbirth. This can create excessive movement and instability in the sacroiliac joints, potentially leading to dysfunction and persistent discomfort.
Trauma
Trauma, such as impacts from falls or vehicle accidents, can injure the sacroiliac joints directly. Such injuries can damage the ligaments that support the joint, leading to misalignment or too much movement (hypermobility). Conversely, it can lead to too little movement (hypomobility) if the body’s response is to stiffen the area. These changes from an original injury can lead to ongoing sacroiliac joint dysfunction.
Symptoms and Diagnosis
In addressing sacroiliac joint fusion, it’s critical to recognize the symptoms of SI joint dysfunction and understand the diagnostic processes involved. We’ll explore the specific indicators of SI joint pain and the tests used to accurately diagnose it.
Identifying SI Joint Pain
Sacroiliac joint pain typically manifests as a sharp, stabbing sensation that may radiate to the lower back, buttocks, groin, or thighs. The discomfort can vary from mild to severe and often increases when standing up from a sitting position or performing weight-bearing activities. Key signs include:
- Back pain: Particularly in the lower back, which may sometimes feel like a deep aching sensation.
- Leg pain: A shooting pain radiating down the leg, often mistaken for sciatica.
- Inflammation: The SI joint might be tender to the touch, indicating inflammation.
- Stability issues: Difficulty maintaining balance due to pain can be a sign of SI joint dysfunction.
- Numbness: In some cases, there might be tingling or numbness in the affected leg.
During a patient’s medical history review, we ask about any incidents that may have triggered the pain, such as a fall or car accident. We also inquire about the duration, intensity, and specific location of the pain, as well as any factors that alleviate or exacerbate it.
Diagnostic Tests
For an accurate diagnosis, we typically start with a thorough physical exam to test for pain triggers and assess the stability of the SI joint. Here are the steps:
Physical Exam:
- Assessment of pain through various maneuvers, like the FABER test, which involves flexion, abduction, and external rotation of the hip.
- Palpation of the SI joint to determine the exact source of pain.
Imaging Tests: These are critical in our diagnostic toolkit.
- X-ray: This can reveal signs of damage or changes in the joint.
- MRI: More detailed than an X-ray, an MRI can detect subtle changes in the joint and surrounding tissues, such as signs of inflammation or damage.
It’s important to note that while imaging tests can provide evidence of potential SI joint dysfunction, they are often used in conjunction with clinical symptoms and the results of a physical exam to confirm a diagnosis.
Non-Surgical Treatment Options
Before considering surgical intervention, we recommend exploring non-surgical treatment options that can provide pain relief and improve function in patients with sacroiliac joint dysfunction.
Physical Therapy
Physical therapy is a cornerstone in the management of sacroiliac joint pain. We aim to strengthen the muscles around the joint, improve flexibility, and enhance stability. Typically, our goals include improving posture and balance, as physical therapists design exercises to specifically target the muscles that support the SI joint.
Medications
The use of medication is often an early step in the treatment protocol for SI joint pain. We rely on over-the-counter pain relievers, like ibuprofen and naproxen, to reduce inflammation and offer pain relief. In cases where the pain is more severe, we may consider prescription strength non-steroidal anti-inflammatory drugs (NSAIDs).
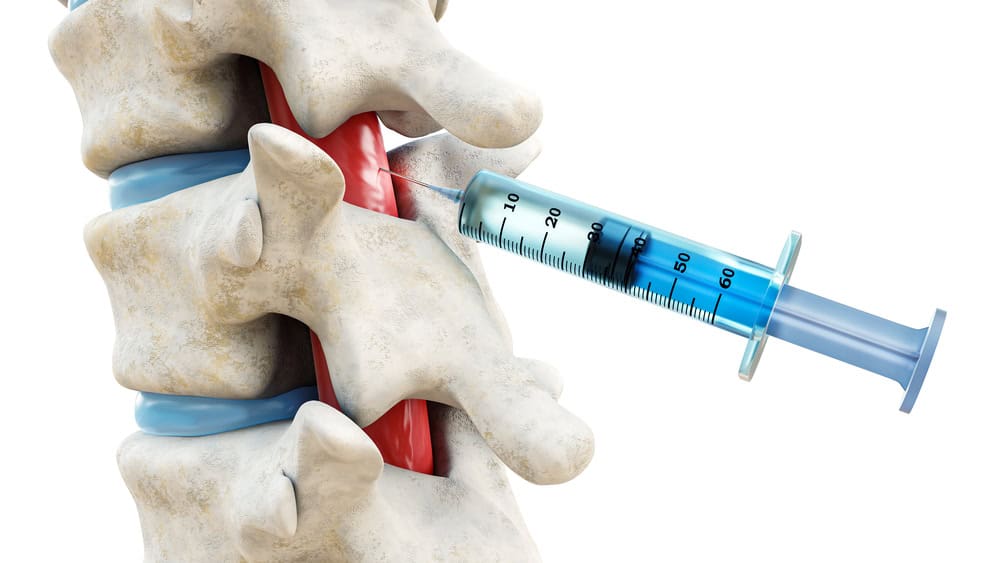
Joint Injections
When physical therapy and medications do not provide adequate pain relief, we explore the option of joint injections. These often include corticosteroid injections combined with a local anesthetic to both diagnose and alleviate pain. We administer injections under fluoroscopic guidance to ensure accuracy. These injections can offer temporary but significant pain relief, allowing patients to participate more effectively in physical therapy.
Sacroiliac Joint Fusion Surgery
Sacroiliac joint fusion surgery is a procedure that aims to alleviate pain caused by SI joint dysfunction. This surgery provides long-term relief by stabilizing the joint and is considered after conservative treatments have failed.
Indications for Surgery
Patients with chronic sacroiliac joint pain that hasn’t responded to non-surgical treatments may be candidates for SI joint fusion. Conditions like sacroiliitis, SI joint inflammation, and degenerative sacroiliitis are common indicators for considering this surgery.
Surgical Techniques
Surgical techniques for sacroiliac joint fusion surgery vary from traditional open surgery to minimally invasive surgery (MIS). The choice of technique depends on the specific case and surgeon preference. Open surgery involves a larger incision and is more invasive, while MIS involves smaller incisions and typically results in faster recovery times and less post-operative pain.
Minimally Invasive SI Joint Fusion
In minimally invasive SI joint fusion, surgeons typically make a small incision and use specialized instruments to place titanium implants and occasionally bone graft material to promote joint fusion. Clinical trials have supported MIS as an effective technique for improving pain and disability associated with SI joint dysfunction.
Post-Operative Care
Following sacroiliac joint fusion surgery, post-operative care is crucial for a successful recovery. Patients receive detailed instructions on activity limitations, pain management, and wound care. The specific recovery protocol will vary, but generally involves physical therapy and gradual return to normal activities.
Risks and Complications
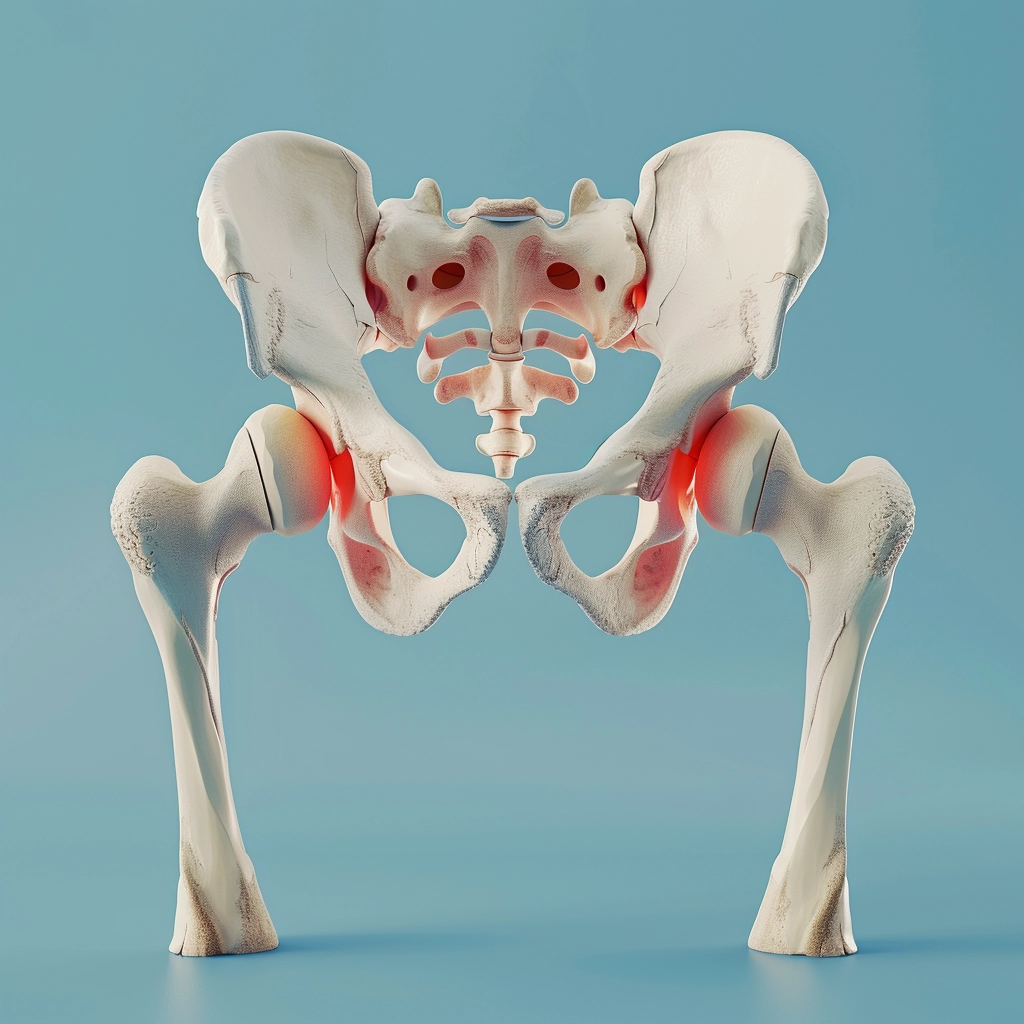
When considering sacroiliac joint fusion, we must be aware of potential risks and complications inherent to the procedure. These include infections, fractures, and issues related to the implants, which may require further medical intervention.
Infections
While sacroiliac joint fusion is typically a minimally invasive procedure, the risk of infections exists, as with any surgical intervention. Signs of infection can include persistent redness, swelling, fever, or pus emanating from the incision site. Our goal is always to minimize this risk through sterile techniques and, when necessary, we may prescribe medication such as antibiotics to combat any infection that arises.
Fracture
Fractures in the pelvic bones can be a rare but serious complication following the surgery. These may result from undue pressure on the bones or a misapplication of the technique during the intervention. Symptoms often include an unexpected increase in pain, which radiates from the site of fracture. If a fracture occurs, we manage it proactively, potentially with bracing, to ensure proper healing.
Implant Issues
Sacroiliac joint fusion typically involves the placement of titanium implants or screws to stabilize the joint. In some cases, these implants can migrate or loosen, leading to discomfort or reduced effectiveness of the fusion. We monitor for mechanical issues with radiographic imaging and are prepared with strategies to address them if they develop. Implant issues might necessitate additional surgeries or, in cases of persistent pain, alternative treatments such as steroid injections to reduce inflammation and manage symptoms.
Recovery and Rehabilitation

In the journey to regain function and manage discomfort after SI Joint Fusion surgery, we emphasize the importance of a structured recovery and rehabilitation plan that addresses both stability and mobility.
Physical Therapy
Physical therapy is a cornerstone of recovery—it promotes the return of strength and flexibility to our sacroiliac joints. A typical physical therapy protocol post-sacroiliac joint fusion includes:
- Pain Management: Use of modalities to control pain and reduce inflammation.
- Range of Motion (ROM): Introducing gentle activities to avoid stiffness while maintaining joint integrity.
- Strengthening Exercises: Gradual incorporation of exercises to improve the support around the pelvis.
Exercise and Activity Modifications
As we progress through healing, modifying daily activities and exercises helps protect the surgical area while enhancing the recovery process. Key considerations include:
Sitting and Standing: Alternating between sitting and standing frequently to prevent undue stress on the sacroiliac joints.
Leg Movements: Avoiding crossing legs or making sudden, sharp movements that could disrupt the integrity of the SI joint area.
Our focus on these modifications aims to foster an environment conducive to healing—balancing the need for rest with the necessity for movement to recover optimally.
Outcomes and Effectiveness

When we consider sacroiliac joint fusion, we aim to assess its effectiveness through meticulous scrutiny. Our focus revolves around tangible outcomes, evidence from research and studies, patient testimonials, and long-term results.
Research and Studies
Extensive clinical trials have provided a strong foundation of evidence supporting sacroiliac joint fusion. For example, a comprehensive review involving 40 patients revealed both significant pain reduction and solid fusion rates. Most patients experienced a marked decline in instability and low back pain, reinforcing the procedure as effective.
Patient Testimonials
In our interactions, patients often share stories of recovery and enhanced quality of life following SI joint fusion. We have noted consistent reports of pain reduction and improved mobility. While individual experiences vary, the sentiment leans positively, contributing to the overall evidence of effectiveness.
Long-Term Results
Looking at the long-term results, Medicare studies and longitudinal data collections underscore the procedure’s sustainability. Rates of solid fusion over the years point to low back pain relief sustaining across time, which implies not only immediate but also enduring benefits for the patients.
Our extensive review underscores the effectiveness of the SI joint fusion technique, with evidence pointing towards tangible improvements in patient outcomes.
Living with SI Joint Fusion

After undergoing an SI joint fusion, our daily lives typically undergo some adaptations. We familiarize ourselves with new routines and pain management strategies tailored to our improved but changed physical state.
Lifestyle Adjustments
The lifestyle adjustments we make post-surgery are crucial for maintaining the success of our sacroiliac joint fusion. Here are some key things to remember:
- Mobility: Initially, we may experience stiffness and reduced mobility. It’s important to adhere to a prescribed physiotherapy plan to regain function.
- Posture: Practicing good posture is essential, especially when standing or sitting for prolonged periods, to prevent stress on the SI joint.
- Activity: We must balance rest with activity. Gradually increasing our levels of activity helps in strengthening the muscles around our sacroiliac joint.
- Lifting: Proper lifting techniques are important to avoid straining the lower back. We should avoid heavy lifting until cleared by our healthcare provider.
Managing Expectations
Understanding and setting realistic expectations play a significant role in living with SI joint fusion:
- Pain Relief: SI joint fusion is aimed at providing pain relief. While some of us may experience significant relief, others might notice a more gradual decrease in pain levels.
- Long-term management: While SI joint fusion can offer relief, it is not a cure-all. We may need to continue with other pain management techniques and lifestyle adjustments.
- Follow-up care: Regular follow-up appointments are essential to monitor our progress and address any concerns.
By recognizing the changes and challenges we may face, we can take proactive steps towards a balanced and comfortable life post-SI joint fusion.
Frequently Asked Questions
In this section, we cover some of the most pressing concerns patients have regarding sacroiliac joint fusion surgery. Our responses draw on current medical insights to give you accurate information.
What is the success rate of sacroiliac joint fusion surgery?
The success rate of sacroiliac joint fusion surgery varies, with studies showing improvement in pain and function for the majority of patients. However, outcomes depend on individual conditions and the criteria for ‘success’ can vary.
What are the potential long-term effects of undergoing an SI joint fusion?
Undergoing SI joint fusion may result in permanent changes, including reduced range of motion in the joint. Long-term benefits often include reduced pain and increased stability.
What is the typical recovery time following a sacroiliac joint fusion procedure?
Recovery times can differ widely, but typically, patients may take several weeks to months to recover from a sacroiliac joint fusion procedure. This includes time for bone fusion, which varies by individual.
Can sacroiliac joint fusion surgery result in permanent restrictions or limit mobility?
Sacroiliac joint fusion surgery can lead to permanent changes in mobility and certain restrictions to prevent stress on the fused joint. However, these limitations are typically balanced with the relief of symptoms.
What are the major pros and cons associated with SI joint fusion?
The pros of SI joint fusion include pain reduction and increased joint stability. The cons may involve potential risks of surgery, such as infection, and the possibility of not achieving the desired outcome.
Which type of medical specialist is qualified to perform sacroiliac joint surgery?
Orthopedic surgeons and neurosurgeons with training in spine surgery are typically qualified to perform sacroiliac joint surgery. It’s essential to choose a provider with experience in SI joint dysfunction.