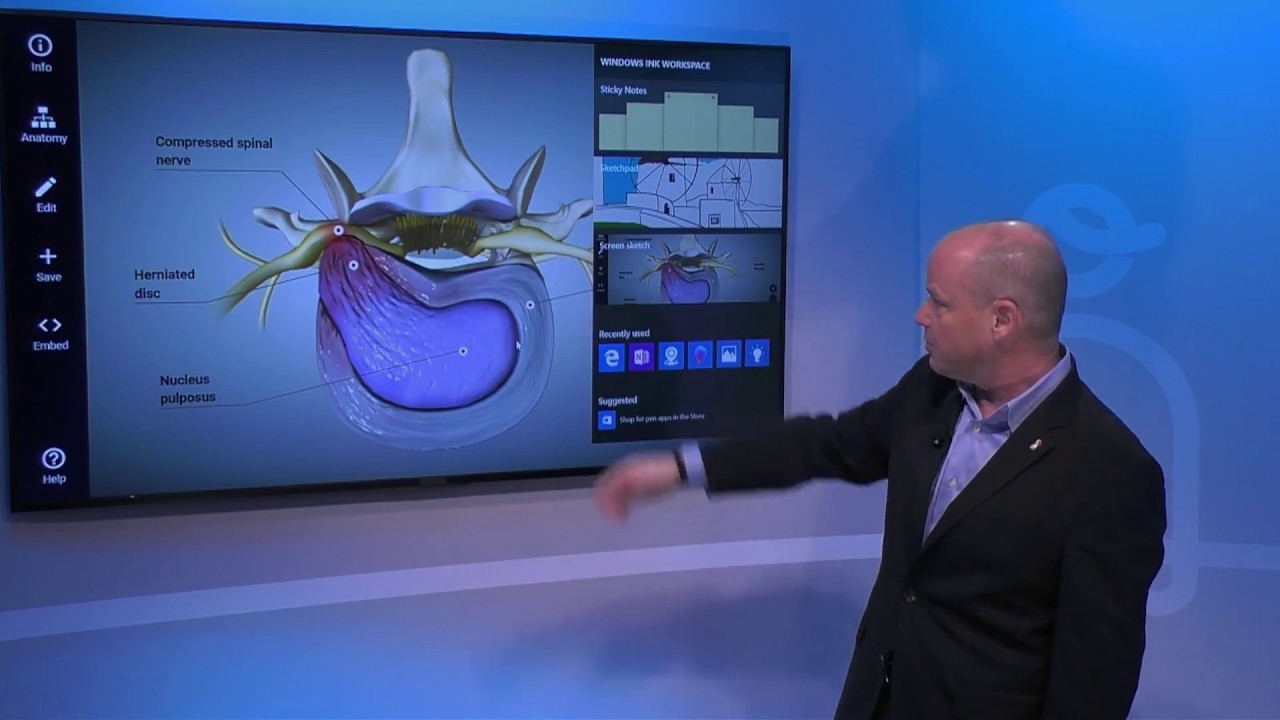
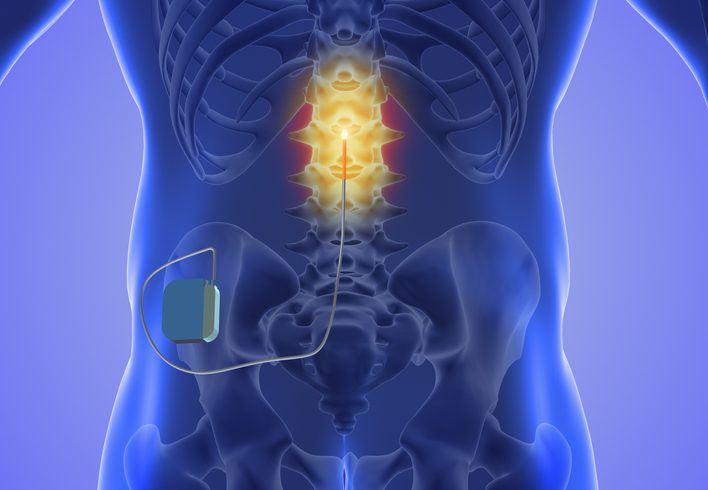
Epidural injections are a medical treatment commonly used to deliver steroids directly into the epidural space in the spine. This procedure is typically sought by patients experiencing inflammation and pain caused by various spinal conditions. The carefully administered steroid can help reduce nerve inflammation and offer pain relief, serving as a nonsurgical approach to managing chronic back pain and discomfort.
The technique for administering an epidural steroid injection involves placing the medication in the epidural space, which is the area outside of the sac of fluid around the spinal cord. This area is rich with nerves that may become inflamed due to irritation from a damaged disc or other inflammatory conditions. By targeting this specific section of the spine, the medications help alleviate localized pain. Our understanding of these procedures is supported by safely guiding patients from the decision-making process through recovery, ensuring that the benefits are maximized while minimizing risks.
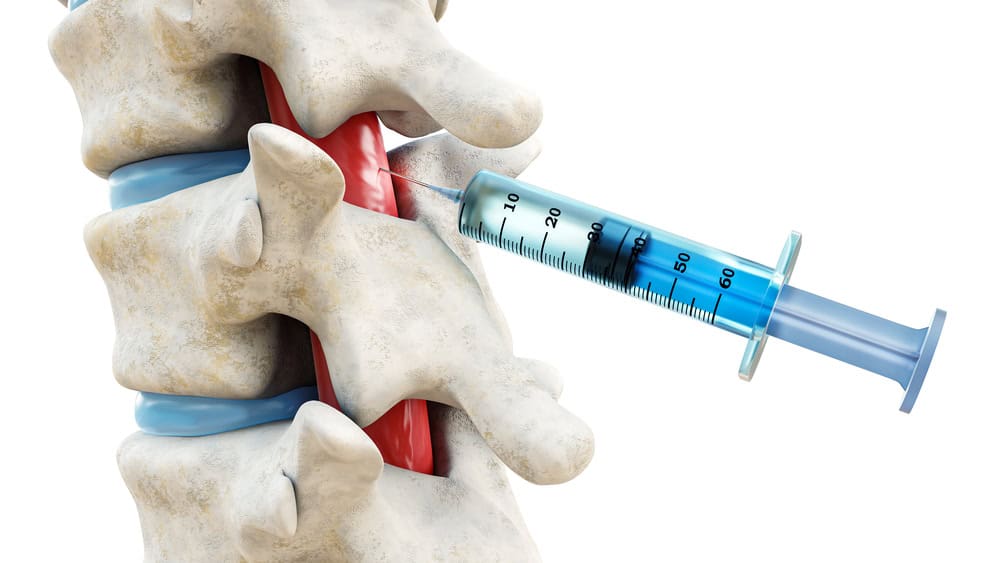
Key Takeaways
- Epidural injections are a pain management option that involve the administration of steroids into the spine.
- The injections aim to reduce nerve inflammation and provide pain relief for a variety of spinal conditions.
- This treatment is part of a broader pain management strategy and must be approached with full understanding of potential benefits and risks.
Understanding Epidural Injections
Epidural injections are a targeted therapy used to provide pain relief by delivering medication directly to the area around the spinal cord. We’ll explore the pertinent anatomy of the spine, the different types of injections available, and how they work to alleviate pain.
Anatomy of the Spine
The spine is a complex structure composed of vertebrae, intervertebral disks, and the spinal cord. Within this configuration, the dura is a protective covering of the spinal cord, creating the epidural space between itself and the bony vertebrae. This space is crucial, as it is the intended target for epidural injections to manage pain.
Types of Epidural Injections
Epidural injections primarily fall into two categories:
- Epidural Steroid Injection (ESI): ESI delivers a corticosteroid with or without a local anesthetic into the epidural space, offering anti-inflammatory benefits to inflamed spinal nerves.
- Epidural Anesthesia: Primarily used during surgery, this involves the injection of anesthetic into the epidural space for numbing purposes.
Each type can be administered via different approaches, including interlaminar (entry through the back of the spinal column) and transforaminal (injection through the side where nerve roots exit the spine) techniques.
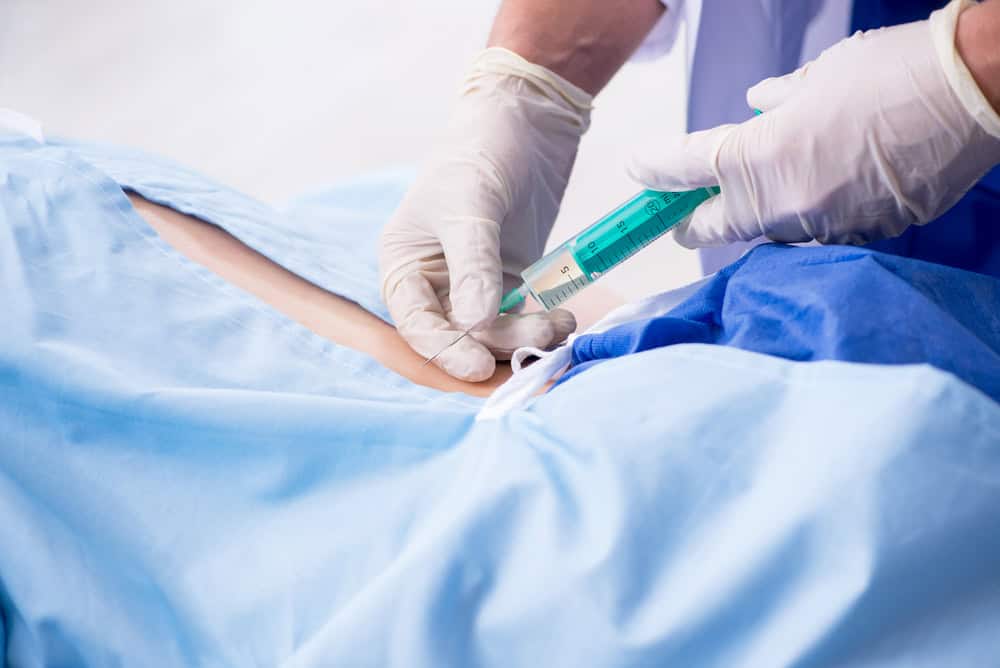
Mechanism of Pain Relief
Epidural injections work by depositing medication directly into the epidural space, which can reduce inflammation and disrupt pain signals from the spinal nerves to the brain. By doing so, these injections provide significant pain relief and are an important part of pain management for conditions causing nerve irritation and inflammation. Corticosteroids act as potent anti-inflammatory agents, while anesthetics can block the transmission of pain signals temporarily.
Indications for Epidural Injections
Epidural injections are a versatile treatment option primarily aimed at offering relief from various types of pain associated with spinal conditions. These injections are specifically formulated to target and alleviate discomfort in distinct areas of the spine.
Common Conditions Treated
We administer epidural injections to treat a range of conditions that cause chronic pain. Some of the most common conditions include:
- Lumbar spinal stenosis: A narrowing of spaces in the lumbar spine, which can put pressure on the spinal nerves.
- Sciatica: Characterized by sharp pain that radiates along the path of the sciatic nerve, typically affecting the back of the legs.
- Herniated disk: Occurs when the soft central portion of a spinal disk bulges out and irritates adjacent spinal nerves.
- Degenerative disk disease: Involves the discs of the spine degenerating or breaking down, leading to pain.
Targeting Specific Pain Areas
Our approach to administering epidural injections aims at localizing treatment to the areas most affected by pain:
- Back pain and leg pain: Injections often focus on the lumbar spine area to reduce inflammation and alleviate pain that extends to the legs.
- Spinal nerves and spinal nerve roots: By targeting these areas with steroids, we aim to decrease the pain caused by nerve root irritation.
Procedure and Techniques
In this section, we’ll explore the specific steps and methods involved in administering epidural injections, focusing on the preparation required, the use of image guidance for accuracy, and the different approaches taken to ensure effective delivery of the medication.
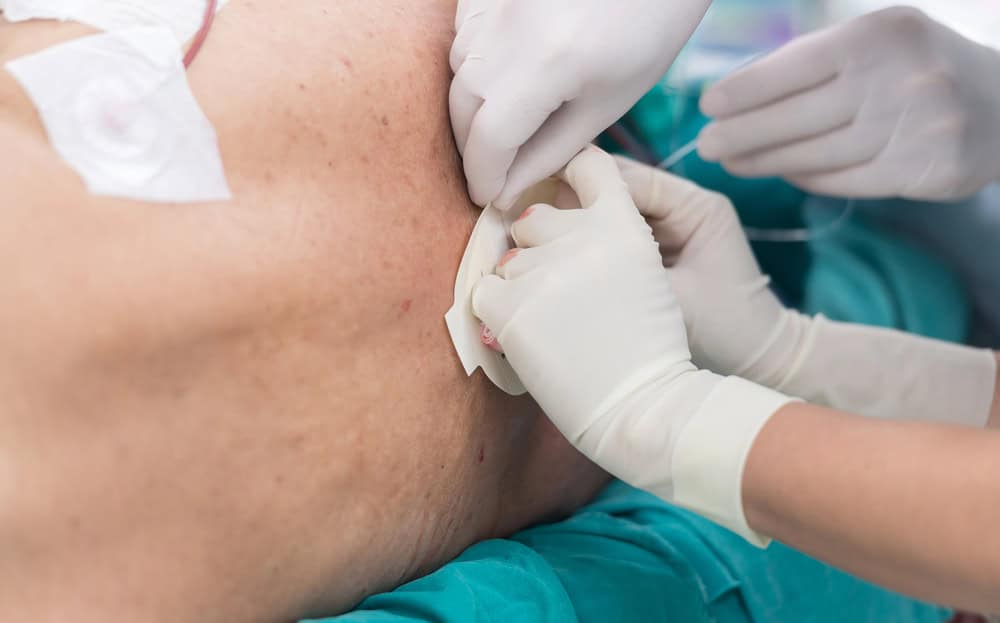
Preparation and Administration
Before performing an epidural injection, we ensure that patients are appropriately prepared. This involves confirming the correct site and the specific condition to be treated. The skin area is cleaned to maintain sterility, and a local anesthetic is often applied to minimize discomfort during needle insertion. The actual procedure is usually done in an outpatient setting, such as a hospital or a specialized clinic.
During the administration, we carefully monitor the patient’s vital signs and pressure in the epidural space to enhance the safety of the procedure and reduce the risks associated with epidural corticosteroid injections. The types of medication used typically include a steroid for its long-term inflammation reduction and sometimes an anesthetic for immediate pain relief.
Image Guidance in Procedures
We often use image guidance when administering epidural injections to increase the accuracy and safety of the procedure. Fluoroscopy is a technique that provides real-time x-ray images, allowing us to visualize the path of the needle and the distribution of the contrast dye. This ensures that the medication is being delivered to the precise area intended for treatment, enhancing the effectiveness and reducing the risk of complications.
Approaches to Injection
There are different techniques we might use for an epidural injection, and the choice usually depends on the specific diagnosis, patient anatomy, and the preference of the healthcare provider.
Interlaminar injection: This traditional approach involves inserting the needle into the back of the epidural space, and it is often employed for a broad distribution of medication.
Transforaminal epidural steroid injection: Alternatively, a more targeted approach is the transforaminal injection, where the needle is placed closer to the affected nerve as it exits the spine.
Lumbar epidural steroid injection: Specifically for lower back pain, a lumbar approach may be used to reduce inflammation and alleviate pain in the lumbar region.
After the procedure, patients may be advised to follow a period of physical therapy to maximize the benefits of the injection. The goal is to achieve pain relief that allows for improved mobility and the ability to participate in daily activities more comfortably. Each technique is performed by trained professionals such as anesthesiologists, physiatrists, or radiologists who specialize in pain management.
Efficacy and Outcomes
When we examine the efficacy and outcomes of epidural injections, our focus centers on their role in pain relief and chronic pain management. We will assess the expected duration of pain relief and how we measure treatment success.
Expected Pain Relief Duration
- Short-term Relief: For many patients, epidural steroid injections provide a reduction in pain for a period that can span from a week up to a few months. Our goal is to provide a window of pain relief during which individuals can engage in physical therapy and rehabilitation, thereby enhancing function and facilitating longer-term healing.
- Long-term Effects: While some patients experience a significant benefit, this therapeutic technique does not guarantee prolonged pain relief for all. We must take a nuanced approach to manage expectations and understand that results may vary, with some cases requiring additional interventions for sustained pain management.
Assessment of Treatment Success
To evaluate the success of these non-surgical treatments, we take a multifaceted approach:
- Pain Scales: We use tools like the Numeric Rating Scale to gauge reductions in pain intensity. Studies have shown no significant difference in outcomes when compared to injections with local anesthetics alone.
- Functionality Assessments: The Oswestry Disability Index helps us measure how the relief translates to improvements in daily activities and overall quality of life.
- Follow-up Evaluations: We conduct follow-up assessments to determine if the epidural steroid injections have had a specific effect on the patient’s pain and function.
When considering epidural injections as a part of pain medicine, we review the evidence, such as research on their long-term effectiveness in older adults, and tailor treatment plans to individual needs for managing chronic pain.
Potential Risks and Side Effects
While an epidural injection can offer significant pain relief, we must consider the potential risks and side effects that could occur. Our focus here is to outline these possibilities to ensure informed decision-making.
Short-term Complications
Infection: Although quite rare, there remains a risk of infection at the injection site, which might result in conditions such as epidural abscess or even meningitis.
Bleeding: There is a possibility of bleeding, especially for those with underlying bleeding disorders.
Discomfort: Discomfort or soreness at the site of injection is common.
Headache: A severe headache may result from spinal fluid leakage, known as a post-dural puncture headache.
Allergies: Allergic reactions to the medication or other substances used during the procedure can occur.
Nerve Damage: Temporary nerve damage can cause numbness, tingling, or weakness in the affected area.
Blood Pressure Drop: Some patients may experience a lightheaded feeling due to a drop in blood pressure.
Injection-related Discomfort: During the procedure, patients may feel pressure or discomfort.
Long-term Complications
Chronic Pain: Chronic pain can be a potential long-term issue, although it is not common.
Inflammation or Irritation: Repeated injections may lead to increased inflammation or irritation in the surrounding tissue.
Diabetes Fluctuations: Patients with diabetes might experience fluctuations in blood sugar levels due to the corticosteroid medication.
Tingling or Paralysis: In extremely rare instances, prolonged tingling or even paralysis can occur due to nerve damage.

In considering epidural injections, we weigh these potential risks against the benefits. Our aim is to provide a clear understanding of what could be expected during and after the procedure.
Post-Procedure Care
After an epidural steroid injection, we focus on two key aspects of post-procedure care: guiding patients through the recovery process and vigilantly monitoring for any adverse effects.
Recovery Process and Guidelines
The first few hours after receiving an epidural steroid injection are pivotal for the recovery process. During this time, it’s crucial to adhere to the following guidelines:
- Rest: We advise patients to rest and avoid strenuous activities for at least 24 hours post-injection.
- Medications: Continue taking your usual medications unless instructed otherwise by your healthcare provider.
- Analgesia: Over-the-counter pain medications may be used to manage any discomfort that occurs once the local anesthetic wears off.
Patients should gradually resume normal activities as tolerated, and some may benefit from physical therapy if recommended by their healthcare provider.
Monitoring for Adverse Effects
While the risk is low, we must be watchful for the following potential adverse effects:
- Infection: Fever, increasing pain, redness, or discharge at the injection site could indicate an infection.
- Bleeding: Any unexpected bleeding or significant bruising around the injection site warrants a call to us immediately.
- Nerve Damage: Persistent numbness, weakness, or tingling sensation may be signs of nerve damage and should prompt a prompt consultation.
- Allergies: In the rare case of an allergic reaction, be alert for symptoms such as rashes, itching, or difficulty breathing.
Patients should reach out to us if they experience increases in swelling, continuing or worsening discomfort, or if there’s a delay in the expected pain relief, as adjustments in their anti-inflammatory therapy or further evaluation may be necessary.
Alternatives and Adjuncts to Epidural Injections
While epidural injections are commonly used for managing pain, especially in the lumbar spine, we acknowledge that they are not suitable for everyone. Patients may seek alternatives due to concerns about side effects, ineffectiveness, or personal preference. We explore both non-invasive and surgical options that can be considered.

Non-Invasive Pain Management Strategies
Non-invasive pain management takes a therapeutic approach that does not break the skin or enter the body. We advocate for physical therapy, as it can strengthen the muscles around the nerves and disks, potentially relieving pain caused by a pinched nerve. Additionally, medications, such as anti-inflammatories or muscle relaxants, can be used in concert to reduce pain and inflammation in the lumbar spine.
Another significant component of non-invasive strategies is body mechanics and ergonomics. We educate patients on posture and lifting techniques which can alleviate stress on the lumbar spine. Hot/cold therapies and electrical stimulation are other modalities that may serve as complementary treatments to further manage pain without the need for invasive procedures.
Surgical Interventions for Pain
When non-surgical treatment is insufficient for pain management, we consider surgical interventions. Surgery might be advisable for those with severe structural issues like herniated disks. Common procedures include discectomy, which involves removing a portion of the disk to relieve pressure on a nerve, and spinal fusion, which entails joining two or more vertebrae to provide stability.
For each patient, surgical risks and benefits need thorough discussion. Surgery is generally reserved for when conservative measures fail and the pain is debilitating or progressively worsening. We work closely with each individual to determine the best course of action based on their unique condition and overall health.

Considerations for Specific Patient Populations
When discussing epidural injections, it’s vital that we consider the unique aspects each patient. From the use of epidural anesthesia during labor to the impact on those with a range of pre-existing conditions, the effectiveness and safety of this procedure can vary significantly.
Epidurals During Labor and Childbirth
Epidural anesthesia is a common choice for pain relief during labor. We, as anesthesiologists, are responsible for managing the delicate balance of providing effective pain management while ensuring the safety of both the mother and the baby. In the context of labor, it’s crucial to tailor the dose and monitor its effect to provide comfort without compromising the mother’s ability to push during childbirth. Crucial concerns involve timing the administration of the epidural and adjusting for factors such as the mother’s pain tolerance and the progress of labor.
- Key Considerations:
- Timing of administration
- Mother’s pain threshold
- Monitoring fetal heart rate
- Adjusting dosages
Impact on Patients with Pre-Existing Conditions
When working with patients with pre-existing conditions such as diabetes, bleeding disorders, or a history of chronic pain or inflammation, we as healthcare providers, including physiatrists, must evaluate the risks and benefits of epidural steroid injections (ESIs). Patients with diabetes may experience challenges with blood sugar management after receiving an ESI, necessitating closer monitoring. For those with bleeding disorders, the risk of hematoma formation is higher, thus requiring careful assessment of the patient’s clotting profile before proceeding. Moreover, for patients suffering from chronic pain due to conditions like herniated discs, the risk-to-benefit ratio of ESIs should be meticulously calculated.
- Pre-Existing Conditions to Account For:
- Diabetes: Impact on blood sugar levels
- Bleeding disorders: Risk of hematoma
- Chronic pain and inflammation: Assessing ESI suitability
By understanding these individualized factors in specific patient populations, we ensure that epidural injections are used safely and effectively, tailored to each patient’s unique needs.
Frequently Asked Questions
In this section, we address common inquiries regarding epidural steroid injections, helping you understand the side effects, treatment efficacy, administration, and alternatives.
What are the potential side effects of epidural steroid injections?
While epidural steroids can be effective for pain relief, they can also lead to side effects such as headaches, sleeping difficulties, anxiety, and temporary increases in blood sugar. Infection, bleeding, and nerve damage are rare but serious risks. Johns Hopkins Medicine provides detailed insights into the potential side effects.
What conditions are treated with epidural injections?
Epidural injections are primarily used to treat conditions causing inflammation of the spinal nerves, such as herniated discs, radiculopathy, degenerative disc disease, and spinal stenosis. These injections are beneficial for both cervical and thoracic spine issues. Information about these conditions is further explained by the Hospital for Special Surgery.
What is the expected duration of relief from an epidural injection?
The duration of pain relief from an epidural injection varies. Some patients may experience relief lasting weeks or months, while for others, the effect can be much shorter. The Cleveland Clinic discusses the variability in pain relief duration.
How are epidural injections for back pain administered?
The administration of an epidural injection involves placing a needle into the epidural space and injecting a steroid medication. This procedure typically takes between 15 to 30 minutes and is performed under local anesthetic. Technique details are outlined by Memorial Sloan Kettering Cancer Center.
What are the success rates of epidural injections for treating spinal stenosis?
Success rates can vary based on the individual condition and severity of symptoms. For spinal stenosis, many patients report significant improvement in pain and function after epidural injections, although these results are not universal.
What alternatives can be considered if epidural injections are ineffective?
If epidural injections do not provide adequate relief, alternatives may include physical therapy, oral medications, or in some cases, surgical intervention. A comprehensive pain management guide can be found at Physicians Group LLC, outlining various options available.