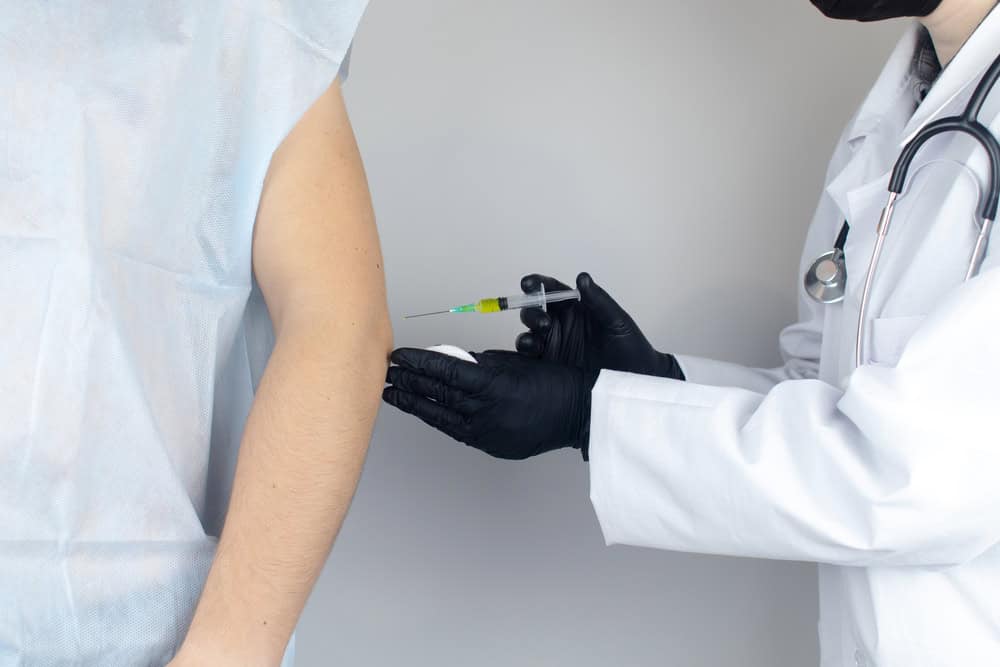
If you are suffering from excruciating abdominal pain due to pancreatic cancer, a celiac plexus block may be the solution. This type of nerve destruction intercepts signals sent by nerves in the abdomen and prevents them from reaching your brain, providing either temporary or long-lasting relief. With this procedure, you can reclaim control over your life and live without agony once more!
What is a Celiac Plexus Block?
To provide relief from chronic pain, a celiac plexus block injection may be administered. This treatment obstructs the signals to the brain sent by the celiac plexus nerves and is classified as a nerve block procedure.
To alleviate the pain experienced by those afflicted with pancreatic cancer or chronic pancreatitis, healthcare providers offer celiac plexus blocks as an effective treatment. This procedure has proven to be successful in offering respite from the intense abdominal discomfort many suffer from these conditions.
- It involves injecting medication around the celiac plexus, which is a network of nerves located behind the abdomen that transmit pain signals from abdominal organs.
- It helps temporarily interrupt pain signals being sent to the brain, providing pain relief.
- It is used to treat chronic pain associated with conditions like pancreatic cancer, chronic pancreatitis, and other cancers that have spread to the abdomen.
- The injection contains a local anesthetic, sometimes mixed with a steroid medication.
- It is performed by an anesthesiologist, pain specialist, or interventional radiologist.
- Pain relief from a celiac plexus block may last for several weeks or months at a time. The procedure can be repeated if pain returns.
- Side effects are usually mild and may include diarrhea, low blood pressure or nausea. Serious complications are rare but could include bleeding, infection or nerve damage.
- It does not treat the underlying cause of the pain but provides symptom relief while other treatments are used for the condition itself.
What is the celiac plexus?
The celiac plexus is an intricate network of nerves located in the upper abdomen, nestled behind the pancreas and astride the body’s primary blood vessel -the mighty Aorta.
Celiac plexus nerves send signals to the brain and spinal cord from digestive system organs, including the:
- Gallbladder.
- Intestines.
- Liver.
- Pancreas.
- Stomach.
What does a celiac plexus block treat?
Healthcare providers rely on a celiac plexus block as an essential treatment for severe abdominal pain caused by cancerous tumors that press against the plexus. Moreover, individuals enduring chronic pancreatitis often turn to this procedure to reduce relentless upper abdominal or back pain due to pancreas swelling.
What distinguishes a celiac plexus block from its advanced form, the neurolytic celiac plexus block (neurolysis)?
To offer temporary respite from discomfort, your medical practitioner may inject steroids or an anesthetic directly into the celiac plexus. This could help relieve pain until it returns – at which time more treatments might be needed depending on the situation. If you have been diagnosed with pancreatitis, this type of therapy is often suggested as a possible solution.
If you are suffering from pancreatic cancer, your doctor may suggest a neurolytic celiac plexus block as treatment. This procedure permanently damages the nerves connected to the celiac plexus by injecting them with an alcohol solution such as ethanol or phenol; this renders these nerves unable to send any pain signals throughout the body. Neurolysis is typically recommended when other treatments have failed and it helps relieve painful symptoms associated with pancreatic cancer.
When will I have a celiac plexus block?
If you are looking for pain relief, a celiac plexus block may be the perfect solution. This outpatient procedure can occur at any stage of pancreatic cancer treatment and is also often used during surgery or endoscopic ultrasound procedures. Your provider will determine if this option is right for your situation.
How should I prepare for a celiac plexus block?
To ensure the best outcome for your procedure, it’s important to follow your healthcare provider’s instructions beforehand. That may include:
- Stop taking certain medicines like blood thinners.
- Fast (not eat or drink) before the procedure. Anesthesia is safer on an empty stomach.
- Cut back on alcohol and quit smoking. These substances increase the risk of complications.
What happens during a celiac plexus block?
A nerve block procedure can take up to one hour, with the injection portion typically completing within minutes. Celiac plexus block is an outpatient treatment and you may return home after it’s done; sending someone along for transportation purposes is among your best options as well as having them remain by your side during that day.
To maximize your comfort, the procedure is usually conducted while you’re in a prone position (lying on your stomach) with a bolster cushion beneath your hips. If it’s too uncomfortable to be in this posture, we can do the treatment when you are lying on your back instead. In addition, an intravenous medication (a sedative) will be administered so that you can relax during the process.
Your healthcare provider will use imaging scans from fluoroscopy X-rays, a CT scan, or an endoscopic ultrasound to guide the procedure.
Your provider:
- Sterilizes the treatment area with an antiseptic and numbs it with a local anesthetic.
- After carefully inserting the needle into your back, a small amount of contrast dye is injected to confirm correct placement. Although you may experience some mild discomfort or feel a slight pinch, this method ensures that the imaging scan will be accurate and reliable.
- After withdrawing the current needle, a new one is used to deliver anesthetics or steroids into the afflicted area in order to reduce nerve pain.
- To achieve a neurolytic procedure, a different needle is used to inject alcohol into the celiac plexus. This injection damages the nerves, thereby eliminating pain signals from reaching the brain.
What happens after a celiac plexus block?
Generally, those who have a nerve block experience relief from their pain in the time frame of 15-30 minutes. It’s still essential to remain at your doctor’s office for an hour or two just to make sure that there are no adverse effects.
Potential side effects may include:
- Bruising, swelling or soreness.
- Infection at the treatment site.
- Diarrhea.
- Low blood pressure.
- Muscle spasms.
What are the potential risks or complications of a celiac plexus block?
Despite being a safe procedure, there are potential risks associated with a celiac plexus block. These may include:
- Allergic reaction to anesthesia or the contrast dye.
- Decreased blood flow to the spinal cord.
- Delayed emptying of stomach contents (gastroparesis).
- Kidney damage or other organ damage.
- Nerve damage.
- Paralysis due to a spinal cord injury.
- Seizures.
What are the benefits of a celiac plexus block?
As many as three-quarters of those who have pancreatic cancer or pancreatitis experience excruciating abdominal pain at the time they receive their diagnosis. This intense agony is likely to affect nearly everyone with these conditions eventually, making a celiac plexus block necessary for most in order to properly manage it.
Healthcare experts usually prescribe potent analgesics to control the pain. However, these pharmaceuticals can result in distressing symptoms including foggy thinking, constipation, and vomiting. With a celiac plexus block treatment you might be able to lower the dosage or frequency of medications needed.
In spite of undergoing medical treatments, more than half of people still endure distressful sensations. Breakthrough pain – which is a stronger experience than common chronic pain – can sometimes occur as well. Thankfully, a celiac plexus block has proven to be an effective way to reduce the frequency of such breakthroughs!
What is recovery like after a celiac plexus block?
Within a day or two after your procedure, you will likely be able to return to the activities of everyday life. However, in order to ensure that you make a full recovery and do not experience any complications, please abstain from driving or engaging in intense physical activity for up to 24 hours following your treatment.
How long does a celiac plexus block provide pain relief?
The alleviation of pain from a nerve block is unique to each person. Generally, most individuals experience 3 to 6 months of relief after receiving a celiac plexus block. If your discomfort returns at any time, you can always opt for another nerve block treatment option.
By inflicting harm to the nerves, a neurolytic celiac plexus block can provide long-term pain relief so that you no longer need to seek treatment.
When should I call the doctor?
You should call your healthcare provider if you experience:
- Dizziness, fainting, unusual thirst (dehydration) or other signs of low blood pressure.
- Shortness of breath.
- Any indicators of infection, including a fever or oozing and reddening around the treated area.
- Tingling, numbness or loss of feeling in the legs.
Pancreatic cancer can take a toll on quality of life due to the severe, chronic pain that it causes. If traditional medications are not providing enough relief or undesirable side effects have surfaced, then celiac plexus block treatment may be helpful in reducing these symptoms. Nerves will be damaged through this procedure so as to prevent them from sending signals of distress and agony to your brain. Consulting with a healthcare professional is recommended for further assessment regarding the potential benefits and risks associated with such treatments.
What conditions typically call for a Celiac Plexus Block?
Celiac plexus blocks are primarily used to help treat abdominal pain related to the following conditions:
- Pancreatic cancer – One of the most common uses is to alleviate pain in patients with unresectable pancreatic cancer. The celiac plexus block can reduce the severe abdominal and back pain associated with this condition.
- Chronic pancreatitis – Abdominal pain from inflammation and damage to the pancreas can be debilitating. A celiac plexus block provides pain relief and improves quality of life for these patients.
- Abdominal cancers – Cancers that have metastasized to the abdomen, such as ovarian, colon, stomach, and liver cancers can cause tumor-related pain that may be eased with a celiac plexus block.
- Chronic abdominal pain – For conditions like irritable bowel syndrome or chronic abdominal pain of unclear cause, celiac plexus blocks can sometimes provide pain relief when other treatments fall short.
- End-stage renal disease – The severe abdominal pain and nausea related to kidney failure and dialysis can sometimes be managed with these nerve blocks.
- Other sources of visceral abdominal pain – Less common causes of abdominal pain originating from organs, such as chronic appendicitis or abdominal aneurysms, may also benefit from celiac plexus blocks.
The procedure is mainly aimed at short-term pain control for chronic abdominal pain conditions. It does not correct the underlying disease process but can improve quality of life. The pain relief duration varies from weeks to months.